OSHA Manual for Dental Office: A Comprehensive Guide (Updated April 15, 2026)
Dental practices must prioritize OSHA compliance, especially regarding infection control, as highlighted by experts like Mary Govoni at Dental Assistant Nation.
The Occupational Safety and Health Administration (OSHA) plays a vital role in ensuring safe working conditions within dental practices; Dentistry presents unique hazards – from infectious diseases and sharps injuries to chemical exposures and aerosol transmission – necessitating strict adherence to OSHA regulations. Understanding these standards isn’t merely about avoiding penalties; it’s about protecting the health and well-being of dentists, dental assistants, hygienists, and administrative staff.
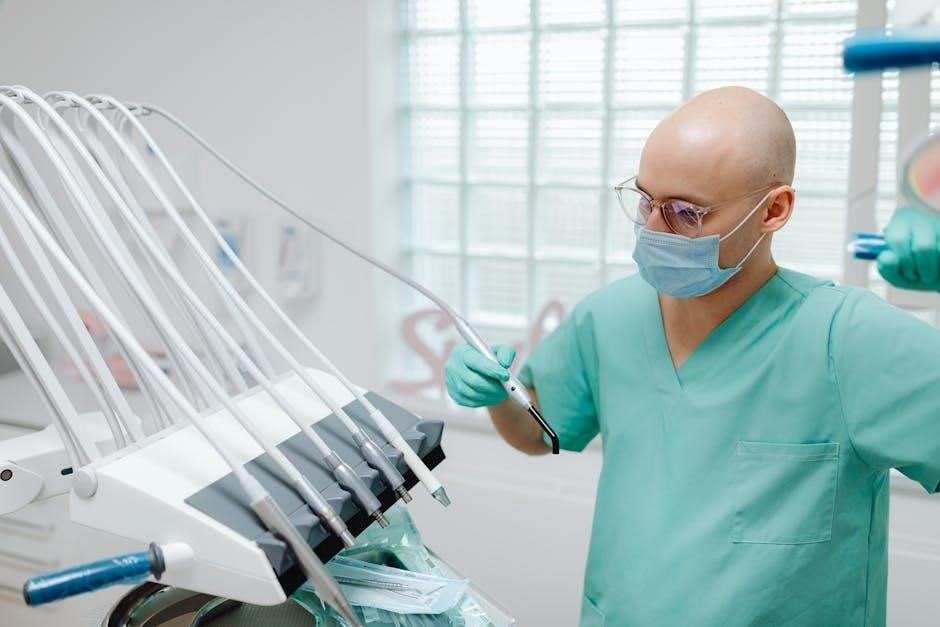
OSHA’s authority stems from the Occupational Safety and Health Act of 1970, mandating employers to provide a workplace free from recognized hazards. In dentistry, this translates to implementing comprehensive programs addressing bloodborne pathogens, hazard communication, personal protective equipment, and respiratory protection. Recent guidance, like that discussed by infection control expert Mary Govoni on Dental Assistant Nation, emphasizes adapting to evolving challenges, such as managing aerosols and preventing COVID-19 transmission.
A proactive approach to OSHA compliance, embodied in a well-maintained manual, is essential for any successful dental practice.
Why an OSHA Manual is Crucial for Dental Practices
An OSHA manual isn’t simply a compliance checklist; it’s the cornerstone of a safe and legally sound dental practice. It demonstrates a commitment to employee safety, minimizing risks associated with infectious diseases, hazardous chemicals, and sharp instruments – all prevalent in dental settings. A comprehensive manual, regularly updated with current guidance (like that from experts featured on Dental Assistant Nation), provides clear protocols for staff to follow.
Beyond legal requirements, a well-defined manual streamlines operations. It ensures consistency in infection control practices, proper handling of regulated waste, and appropriate use of personal protective equipment. This consistency reduces the likelihood of errors and potential exposures.
Furthermore, a readily available manual proves invaluable during OSHA inspections, showcasing a proactive approach to safety and potentially mitigating fines. It’s a vital tool for training new employees and reinforcing best practices for the entire team, fostering a culture of safety.
Core OSHA Standards for Dental Offices
Dental offices face specific OSHA regulations, including Bloodborne Pathogens, Hazard Communication, PPE, and Respiratory Protection.
Bloodborne Pathogens Standard (29 CFR 1910.1030)
The Bloodborne Pathogens Standard is paramount in dentistry due to constant exposure to blood and other potentially infectious materials (OPIM). This OSHA regulation (29 CFR 1910.1030) mandates a comprehensive program to protect employees from Hepatitis B Virus (HBV), Human Immunodeficiency Virus (HIV), and other bloodborne pathogens.
Key components include developing an Exposure Control Plan (ECP), outlining procedures for handling infectious materials, implementing engineering controls like sharps containers and dental dams, providing appropriate Personal Protective Equipment (PPE) – gloves, masks, eye protection – and offering Hepatitis B vaccination free of charge to all at-risk employees.
Furthermore, proper sharps disposal, hand hygiene, and post-exposure protocols are crucial. Detailed recordkeeping of training, vaccinations, and exposure incidents is also required. Regular review and updates to the ECP are essential to maintain compliance and employee safety.
Hazard Communication Standard (29 CFR 1910.1200)
The Hazard Communication Standard (HazCom), outlined in 29 CFR 1910.1200, ensures dental staff understand the risks associated with chemicals used daily. This standard, often referred to as “Right-to-Know,” requires a written program detailing how the practice manages and communicates chemical hazards.
Crucially, a comprehensive chemical inventory must be maintained, alongside readily accessible Safety Data Sheets (SDS) for each product. These SDSs provide vital information on chemical composition, hazards, safe handling procedures, and emergency measures.
Proper labeling of containers is also essential, clearly identifying the chemical and its associated hazards. Employee training on HazCom, including SDS interpretation and safe chemical handling, is mandatory. This includes understanding appropriate PPE when working with specific chemicals, like disinfectants and sterilants. Regular program review and updates are vital for continued compliance and a safe work environment.
Personal Protective Equipment (PPE) Standard (29 CFR 1910.132)
The Personal Protective Equipment (PPE) Standard, 29 CFR 1910.132, mandates dental practices provide and ensure the use of appropriate PPE to protect employees from workplace hazards. A thorough hazard assessment is the first step, identifying potential exposures like bloodborne pathogens, aerosols, and chemical splashes.
Based on this assessment, the practice must select and provide suitable PPE, including gloves, masks, eye protection (goggles or face shields), and protective clothing. Employee training on proper PPE donning, doffing, use, limitations, and maintenance is crucial.
Furthermore, the practice must establish and enforce PPE usage policies. Regular inspection and replacement of damaged or ineffective PPE are essential. Hand hygiene protocols must complement PPE use. Maintaining a readily available supply of appropriate PPE is vital for consistent protection and compliance with OSHA regulations.
Respiratory Protection Standard (29 CFR 1910.134)
The Respiratory Protection Standard (29 CFR 1910.134) is critical in dentistry due to aerosol-generating procedures. A written respiratory protection program is required, outlining procedures for selection, fit testing, medical evaluations, and proper respirator use.
Dental practices must determine if respirators are necessary where airborne contaminants exceed permissible exposure limits. N95 respirators are commonly used, but proper fit testing is mandatory to ensure a secure seal. Employees must undergo a medical evaluation to confirm they can safely wear a respirator.
Training must cover proper donning, doffing, storage, cleaning, and maintenance. The program should detail procedures for filter replacement and respirator inspection. Regular program review and updates are essential to maintain compliance and protect employees from inhaling hazardous airborne particles.
Developing Your Dental Office OSHA Program
Creating a robust OSHA program involves detailed plans for exposure control, hazard communication, and meticulous recordkeeping – essential for a safe dental environment.
Exposure Control Plan (ECP) – Key Components
The Exposure Control Plan (ECP) is the cornerstone of OSHA compliance in a dental setting. It’s a written document detailing how the practice will minimize or prevent employee exposure to infectious materials, specifically bloodborne pathogens.
Key components include: a detailed evaluation of workplace exposure risks, specifying job tasks and procedures involving potential exposure. Methods for minimizing exposure, such as engineering controls (sharps containers, ventilation), work practice controls (hand hygiene, proper instrument handling), and Personal Protective Equipment (PPE) selection must be clearly outlined.
Furthermore, the ECP must address post-exposure procedures, including immediate first aid, reporting protocols, and access to necessary medical evaluations and follow-up. Regular review and updates – at least annually, or when changes occur – are crucial to maintain its effectiveness. Employee training on the ECP is mandatory, ensuring everyone understands their roles and responsibilities in preventing exposure. A well-defined ECP demonstrates a commitment to employee safety and minimizes legal risks.
Written Hazard Communication Program
A comprehensive Written Hazard Communication Program is essential for complying with OSHA’s Hazard Communication Standard. This program ensures employees understand the hazards associated with chemicals used in the dental office, like disinfectants, sterilants, and etching agents.
The program must include: a detailed inventory of all hazardous chemicals, readily accessible Safety Data Sheets (SDS) for each chemical, and clear labeling of containers. Employee training is paramount, covering how to interpret SDS information, understand chemical hazards, and implement appropriate safety measures.
Crucially, the program should outline procedures for handling spills, leaks, and emergencies involving hazardous chemicals. Regular updates are necessary to reflect any new chemicals introduced or changes in SDS information. Maintaining a well-organized and accessible program demonstrates a proactive approach to chemical safety and protects both employees and patients from potential harm. This program is a vital component of a robust OSHA manual.
Recordkeeping Requirements (380 Logs)
OSHA mandates meticulous recordkeeping for dental offices, primarily utilizing OSHA Form 300, 300A, and 301 – often referred to as “380 Logs.” These logs document work-related injuries and illnesses, enabling tracking of safety trends and identifying areas for improvement.
Specifically, the OSHA 300 Log records details of each incident, including employee name (protected), injury/illness description, cause, and job title. Form 300A is an annual summary of the 300 Log, posted prominently from February 1st to April 30th each year. Form 301 provides a more detailed investigation report for each individual incident.
Maintaining accurate and complete records is critical during an OSHA inspection. Records must be retained for five years. Proper recordkeeping demonstrates a commitment to employee safety and helps proactively address potential hazards, contributing to a safer dental practice environment.

Specific Dental Office Hazards & Controls
Dental offices face unique risks, including aerosol transmission, sharps injuries, and chemical exposures. Implementing robust controls is vital for employee and patient safety.
Aerosol Management and COVID-19 Considerations
Aerosol-generating procedures (AGPs) are inherent in dental practice, creating a significant pathway for potential airborne pathogen transmission. Managing these aerosols is paramount, especially considering ongoing concerns related to COVID-19 and other respiratory illnesses. Effective control measures include utilizing high-volume evacuation (HVE) systems, rubber dams where feasible, and strategically positioning patient positioning.

Ventilation plays a crucial role; increasing air exchanges per hour and considering air purification systems with HEPA filters can substantially reduce airborne concentrations. Regular maintenance and monitoring of ventilation systems are essential. Furthermore, appropriate personal protective equipment (PPE), including N95 respirators, is vital for dental personnel during AGPs.
Screening protocols for patients, alongside strict adherence to hand hygiene and surface disinfection, remain critical components of a comprehensive aerosol management strategy. Staying updated with the latest guidance from OSHA and the CDC is also necessary to adapt to evolving recommendations.
Sharps Injury Prevention
Needlestick injuries and sharps-related cuts pose a serious risk of bloodborne pathogen transmission in dental settings. A robust sharps injury prevention program is therefore non-negotiable. This program must encompass several key elements, beginning with the utilization of safety-engineered devices (SEDs) whenever possible – needles with retractable shields, for example.
Proper disposal of sharps is equally critical. Clearly labeled, puncture-resistant sharps containers must be readily accessible in all areas where sharps are used. Employees require comprehensive training on safe sharps handling, including proper disposal techniques and procedures for reporting injuries.
Post-exposure protocols must be clearly defined and readily available. Immediate washing of the wound, reporting the incident, and seeking prompt medical evaluation are essential steps. Maintaining detailed records of all sharps injuries is also a regulatory requirement;
Chemical Hygiene Plan – Disinfectants & Sterilants
Dental practices utilize a wide array of chemicals, demanding a comprehensive Chemical Hygiene Plan. This plan must detail procedures for safely handling disinfectants, sterilants, and other hazardous chemicals. Crucially, it requires a thorough inventory of all chemicals present, accompanied by readily accessible Safety Data Sheets (SDS).
Employee training is paramount, covering proper chemical handling, storage, and disposal. Understanding dilution ratios, contact times, and potential hazards is essential. The plan should also address spill control procedures and the availability of appropriate personal protective equipment (PPE).
Regular review and updates are vital to ensure the plan remains current with evolving regulations and best practices. Proper ventilation and labeling of chemical containers are also key components of a compliant and safe dental environment.
Waste Management (Biohazardous & Regulated Medical Waste)
Proper waste management is a cornerstone of dental OSHA compliance, specifically concerning biohazardous and regulated medical waste. A detailed plan must delineate procedures for segregating, handling, and disposing of these materials according to federal, state, and local regulations.
Sharps containers – puncture-resistant, leak-proof, and properly labeled – are essential for safely discarding needles, blades, and other sharp instruments. Contaminated waste, such as extracted teeth, blood-soaked materials, and impression materials, requires specific disposal protocols.
Employee training must cover waste segregation, container usage, and spill cleanup procedures. Maintaining accurate records of waste disposal is also crucial. Partnering with a licensed medical waste disposal company ensures compliant and safe removal from the dental facility.
Training and Documentation
Comprehensive training and meticulous documentation are vital for a successful OSHA program in dentistry, ensuring employee safety and demonstrating compliance.
Annual OSHA Training Requirements
Maintaining current OSHA training is non-negotiable for all dental personnel. Yearly updates are crucial, covering Bloodborne Pathogens, Hazard Communication, PPE, and Respiratory Protection – the core standards impacting dental practices. This isn’t a one-time event; it’s a continuous process.
Training must be specific to the workplace, detailing the dental office’s Exposure Control Plan (ECP) and hazard communication protocols. Documentation of each training session is paramount, including dates, attendees, topics covered, and trainer qualifications.
Refresher courses should address any policy changes, new equipment, or emerging hazards like evolving COVID-19 protocols. Consider utilizing online modules, in-person sessions, or a blended approach to cater to diverse learning styles. Verification of understanding through quizzes or practical demonstrations is highly recommended. Proper record-keeping demonstrates due diligence during potential OSHA inspections.
Employee Medical Evaluations
OSHA mandates medical evaluations for employees potentially exposed to occupational hazards, particularly bloodborne pathogens and respiratory risks. This includes baseline evaluations before starting work and periodic follow-ups, as determined by risk assessment.
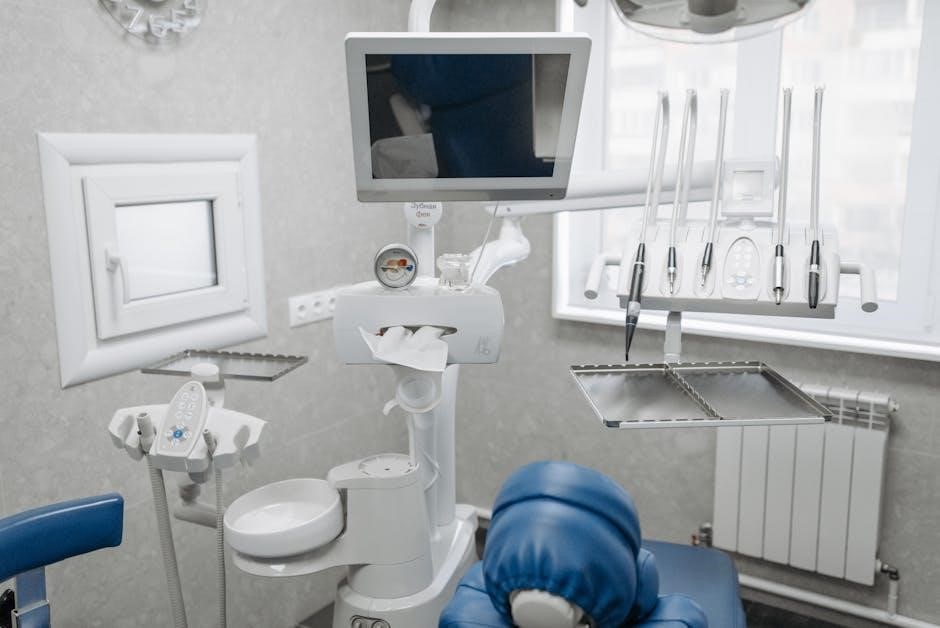
Hepatitis B vaccination is a cornerstone of these evaluations. Employees must be offered the vaccine free of charge, and declination must be documented. Medical evaluations also assess an employee’s ability to use respirators safely, including fit testing and medical questionnaires.
Confidentiality is paramount; medical records must be maintained separately from personnel files. Evaluations should be conducted by a licensed healthcare professional. Documentation of all evaluations, vaccinations, and fit testing results is essential for demonstrating compliance. These records are vital during OSHA inspections and demonstrate a commitment to employee health and safety.
Maintaining Accurate Records & Documentation
Comprehensive recordkeeping is fundamental to a successful OSHA program in a dental office. This includes maintaining the Exposure Control Plan (ECP), Hazard Communication Program, and training records for all employees. Detailed documentation of Hepatitis B vaccinations, respirator fit testing, and medical evaluations is crucial.
Sharps injury logs (380 Logs) must be meticulously maintained, detailing the incident, device involved, and follow-up procedures. Chemical Safety Data Sheets (SDS) must be readily accessible to employees. Regular audits of these records are essential to ensure completeness and accuracy.
Records should be retained for the duration specified by OSHA regulations – typically three years. Proper organization and easy retrieval are vital during an OSHA inspection. Digital recordkeeping systems can streamline this process, but ensure data security and backup procedures are in place. Accurate records demonstrate a proactive approach to safety and compliance.
OSHA Inspections & Compliance
Be prepared for potential OSHA inspections; understanding common citations in dental offices is key. Proactive compliance, utilizing resources like OSHA’s website, is vital.
What to Expect During an OSHA Inspection
An OSHA inspection typically begins with an opening conference where the Compliance Safety and Health Officer (CSHO) will explain the reason for the inspection and the scope. Expect a thorough walk-through of the dental practice, focusing on areas with potential hazards – operatories, sterilization areas, and laboratory spaces.
The CSHO will observe work practices, review your OSHA program documents (like the Exposure Control Plan and Hazard Communication Program), and request records such as training logs, medical evaluations, and 380 logs. Employees will likely be interviewed privately to gather information about safety procedures and any concerns they may have.
Documentation is crucial; having a well-maintained OSHA manual readily available demonstrates a commitment to safety. Be prepared to answer questions about your procedures for bloodborne pathogens, hazard communication, PPE, and waste management. The inspection concludes with a closing conference where preliminary findings are discussed. A written report will follow, outlining any citations and required corrective actions.
Common OSHA Citations in Dental Offices
Dental offices frequently face citations related to Bloodborne Pathogens (29 CFR 1910.1030). These often involve incomplete or missing Exposure Control Plans, inadequate sharps container usage, and insufficient training on infection control protocols. Hazard Communication (29 CFR 1910.1200) is another common area of concern, with violations stemming from unlabeled chemical containers or a lack of Safety Data Sheets (SDS).
Personal Protective Equipment (PPE) deficiencies – like not providing appropriate gloves, masks, or eye protection – also lead to citations. Recordkeeping errors regarding 380 logs (injury and illness records) are frequently noted. Furthermore, failing to provide required medical evaluations, such as Hepatitis B vaccinations, can result in penalties.
Aerosol management deficiencies, particularly relevant post-COVID-19, are increasingly scrutinized. Proactive compliance through a comprehensive OSHA manual and diligent adherence to standards is vital to avoid these common pitfalls and ensure a safe work environment.
Resources for Staying Compliant (OSHA Website, Dental Associations)
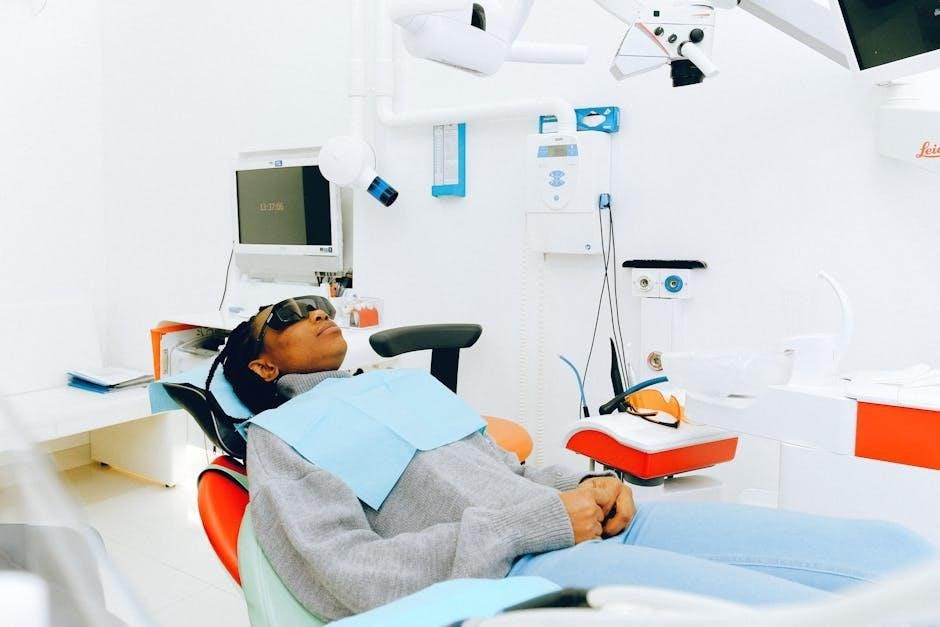
The official OSHA website (osha.gov) is the primary source for regulations, interpretations, and compliance assistance materials. It offers downloadable guides, fact sheets, and access to eTools for various industries, including dentistry. Dental associations, such as the American Dental Association (ADA) and state-level dental societies, provide valuable resources tailored specifically to dental practice needs.
These associations often offer OSHA compliance courses, customizable exposure control plan templates, and updates on regulatory changes. Organizations like the Dental Infection Control Training (DICT), featuring experts like Mary Govoni, provide specialized training and guidance. Consulting with OSHA compliance experts can also ensure your practice meets all requirements.
Regularly reviewing these resources and participating in continuing education is crucial for maintaining a safe and compliant dental office. Staying informed minimizes risks and demonstrates a commitment to employee well-being.
